People using opioids for long-term pain urged to join study to improve patient care
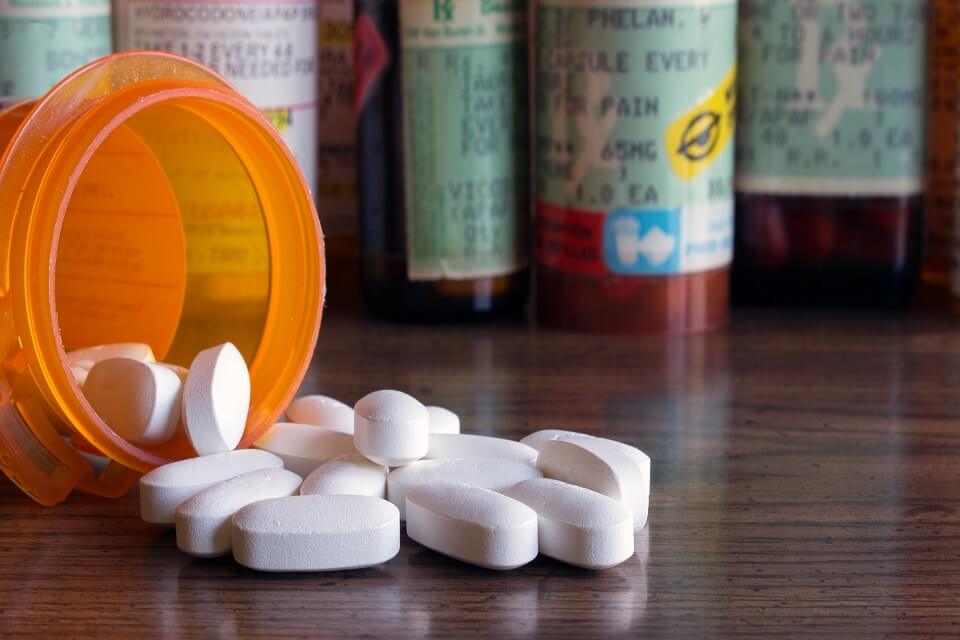
Researchers at Keele University have launched an innovative study to improve care for patients who manage long-term pain using opioids.
The study forms part of a five-year research programme called PROMPPT, which is funded by the National Institute for Health Research (NIHR), and comes as the NHS aims to tackle overprescribing of opioids, with a recent Public Health England report finding too many patients become dependent on these medicines.
Prescriptions for these medicines in England and Wales have risen dramatically from more than 14 million in 2008 to 23 million in 2018. But although opioids can be effective painkillers for short-term pain, for many people they do not help in the long-term and can cause other problems.
Louise Trewern has lived with pain for most of her adult life. She said: “I used opioids for over 12 years. At first, they helped me to cope better and to carry on looking after my children and running my home.”
But the benefits Louise experienced were not long-lasting, and she noticed several side-effects of using opioids for such a long time.
She said: “Even on the opioids my pain would get worse and my dose was increased. That worked for a while, until it didn’t, and then my dose would be increased again. At the same time, my skin condition became worse, a cold would put me in bed for a week and I put on weight. I nodded off in the day, even in the middle of a video-call with my grandson but I couldn’t sleep at night. Taking part in this research is an amazing opportunity for me and others like myself who live with pain to improve the care that we receive.”
One issue is that many people using opioids do not always know about their morphine-like properties and the risks associated with long-term use.
“Many people do not realise that their pain medicines are opioids,” said Dr Sarah Harrisson, a specialist pain physiotherapist at Keele University and a research associate on the PROMPPT study.
To combat this, the research team has created a short animation explaining which medicines are opioids and which are not, with Dr Harrisson adding: “Information about whether painkillers are opioids or not has not always been readily available to people. We hope the video we have developed will help make this information more accessible.”
The research team is now keen to hear from people with long-term pain who are willing to share their experiences and views on using opioid medicines for their pain. To help them learn from as many different people as possible, the research team has set up an online discussion forum called the Q-PROMPPT Blog so that participants can take part via the internet how and when they want to. The blog has been designed so that people with basic computer skills with no experience of using discussion forums can fully participate.
One area the Q-PROMPPT Blog will discuss is the healthcare and support that people living with long-term pain receive. A recent report recommends that more clinical pharmacists work as part of the team in GP surgeries and play a greater role in looking after people with long-term health problems. Clinical pharmacists have done extra training in patient care and are well placed to contribute to the care of people living with long-term pain.
Dr Julie Ashworth, Senior Lecturer in Pain Medicine at Keele’s School for Primary, Community and Social Care co-leads the PROMPPT programme and said: “By really understanding the views of people with experience of long-term pain and using opioid painkillers through the online blog we can develop a clinical pharmacist review that is relevant, useful and appealing to the people who will use it. Too often, people with long-term pain struggle to find the help they need and this study is a great opportunity for their voice to be heard.”
The findings from the study will be combined with the results of interviews with patients and healthcare professionals, which will be used to help design a new way for clinical pharmacists to review patients taking long-term opioids; help them to reduce or stop opioids if appropriate; and to support them to live well with long-term pain.
Health Secretary Matt Hancock said: “We are in the grip of an over-medication crisis and it is vital that we help people find alternatives to addictive opioids to manage their pain. This government-funded study will help pharmacists and health professionals better support their patients and help move them onto more effective treatments.
“Prescribed drugs have an important role to play. But we know that many people are becoming dependent on drugs that have long since stopped working for them. Yet they are being prescribed against clinical guidelines.
“We have seen in the United States the devastation that is caused by opioid addiction – we cannot and will not allow that to happen in this country and I urge anyone eligible to participate in this vital research.”
The blog has been launched today (Thursday 3 October, 2019) and participants need to register in order to take part, and can sign up by visiting www.promppt.co.uk.
For more information about the study and to find out how to take part, visit www.promppt.co.uk and follow @KeelePain on Twitter and Facebook.
Most read
- Keele-led partnership to lead multi-million pound research initiative to transform mental health support
- New debate series to explore societal challenges affecting universities
- Keele researchers selected for prestigious USA exchange programme
- Keele University launches pioneering green hydrogen generation hub
- Keele celebrates graduation of its first fully qualified paramedics
Contact us
Andy Cain,
Media Relations Manager
+44 1782 733857
Abby Swift,
Senior Communications Officer
+44 1782 734925
Adam Blakeman,
Press Officer
+44 7775 033274
Ashleigh Williams,
Senior Internal Communications Officer
Strategic Communications and Brand news@keele.ac.uk.



