New surgery for groin pain found to be more effective than physiotherapy
As the FIFA World Cup approaches, researchers have found that keyhole surgery could help get injured footballers back on the pitch faster than physiotherapy-led treatments.
Researchers from Keele University’s Research Institute for Primary Care and Health Sciences worked with colleagues at the Universities of Warwick and Bristol to analyse two treatments for femoroacetabular impingement (FAI) syndrome, a cause of hip pain that is most common in young adults and people who do sports.
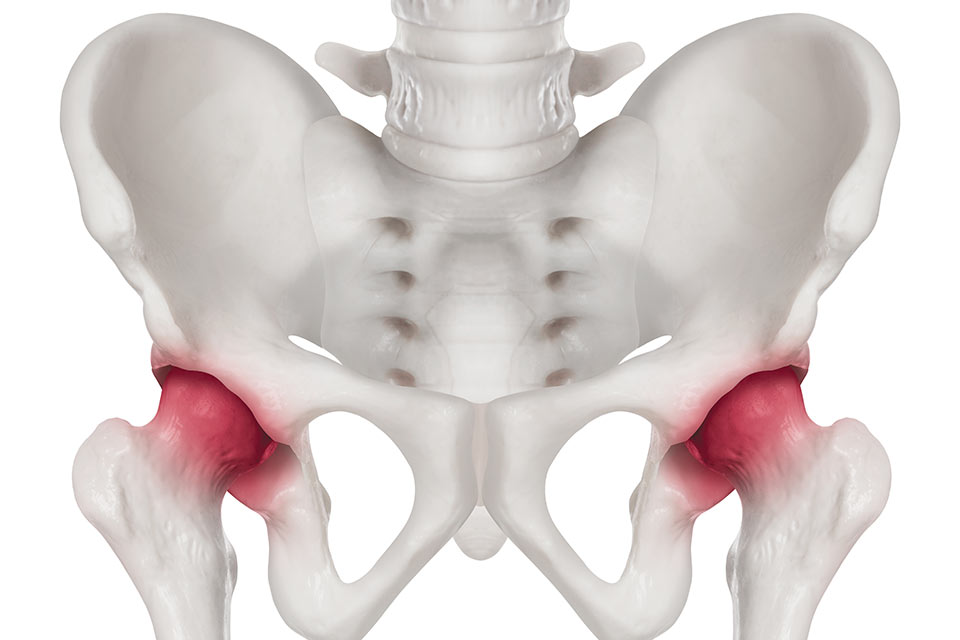
FAI syndrome is due to a problem with the hip’s ball and socket joint. In some people the ball is more egg shaped than round which can cause it to rub unevenly against the socket. This causes damage to the delicate cartilage that lines the socket and is especially debilitating for active people; as the damage accumulates, their pain gets worse causing loss of movement.
The research is the world’s first randomised trial to highlight the benefit of hip arthroscopy, a new treatment for FAI syndrome. Hip arthroscopy, a keyhole surgery procedure, can be used to repair the damage to the hip and to reshape the ball to make it round again.
NIHR Professor Nadine Foster, Professor of of Musculoskeletal Health at Keele University, said: “This trial compared a high quality physiotherapy exercise intervention versus hip surgery, and the results show that both groups of patients improved over 12 months, but that those who had the surgery had, on average, better results in terms of reduced hip pain and hip-related quality of life.”
NIHR Professor Foster, who led the physiotherapy intervention trials, added: “The difference between the groups in hip-related quality of life is clinically meaningful although there were no differences in general health-related quality of life. In addition the cost analysis highlighted that, at least at 12 months, the surgery was associated with much higher costs than the physiotherapy-led personalised hip therapy. The team are following patients up at longer term points to see if the differences are sustained and to find out if the cost effectiveness of surgery compared to physiotherapy changes over three years and longer.”
Professor Damian Griffin, Professor of Trauma and Orthopaedic Surgery at University of Warwick, said: “Now hip surgeons like myself who specialise in looking after young active people are turning our attention to identifying the people who are most likely to benefit from hip arthroscopy. We want to work out how to help these people recover in the shortest possible time, getting them back to work, everyday life without pain, and their sport.”
The team’s clinical trial was held over five years and involved the collaboration of 23 hospitals in the UK. Between July 2012 and July 2016 they recruited 348 participants; they randomly allocated 171 participants to receive hip arthroscopy and 177 were randomly allocated to receive personalised hip physiotherapy programmes.
They compared the effectiveness of the new treatment to physiotherapy-led programmes and found that patients improved with both treatments but were significantly better a year later after hip arthroscopy. Their new research paper, Hip arthroscopy versus best conservative care for the treatment of femoroacetabular impingement syndrome (UK FASHIoN): a multicentre randomised controlled trial is published in The Lancet.
Most read
- Keele-led partnership to lead multi-million pound research initiative to transform mental health support
- New debate series to explore societal challenges affecting universities
- Keele researchers selected for prestigious USA exchange programme
- Keele University launches pioneering green hydrogen generation hub
- Keele celebrates graduation of its first fully qualified paramedics
Contact us
Andy Cain,
Media Relations Manager
+44 1782 733857
Abby Swift,
Senior Communications Officer
+44 1782 734925
Adam Blakeman,
Press Officer
+44 7775 033274
Ashleigh Williams,
Senior Internal Communications Officer
Strategic Communications and Brand news@keele.ac.uk.



