Biography
After obtaining a BSc (Hons) in Biochemistry at Leeds University, I obtained my PhD at Keele in 1991 whilst training as a Clinical Biochemist at what is now the University Hospital of North Midlands NHS Trust (UHNM). I obtained my professional qualifications with the Royal College of Pathologists, gaining Membership (MRCPath) in 2000 and Fellowship (FRCPath) in 2008.
Having worked my way up the clinical and academic ladders, I was appointed Head of Clinical Biochemistry at UHNM in 2004 and Honorary Professor of Clinical Biochemistry at Keele in 2008. Along the way, in 1999 I was awarded the Professors’ Prize, a research prize, sponsored by the UK Heads of Academic Clinical Biochemistry Departments, awarded for 'outstanding scientific contribution to Clinical Biochemistry by a person under the age of 40'. In my professional role, I served on a number of committees for both the Association for Clinical Biochemistry and Royal College of Pathologists. I also served as Director of Research and Innovation at UHNM from 2013-2020.
Having retired from my clinical role within the NHS in 2020, I am now based at Keele University where my clinical research interests focus on clinical laboratory testing, particularly with respect to diabetes, endocrinology and mental health. Despite this quantitative applied clinical research focus, I have more recently developed a passion for lived experience after becoming a volunteer at Expert Citizens CIC (https://expertcitizens.org.uk/) in 2019. It was here that I saw the potential of the Expert Citizens Insight Evaluation framework (https://expertcitizens.org.uk/insightevaluation/) for promoting quality improvement in public and patient involvement in the health and social care research.
Now a Non-Executive Director at Expert Citizens, I led on obtaining funding for the initial phases of the joint Keele/ Expert Citizens Insight | Public Involvement Quality Recognition and Awards programme. A Health Foundation’s Q Community member with training in both clinical research and quality improvement, I now have a rapidly growing passion for promoting lived experience in health and social care research.
Academically, I have published over 230 peer-reviewed papers including several in the Lancet and British Medical Journal, with a h-index of 64 (https://www.researchgate.net/profile/Anthony-Fryer/scores) and a Research Intertest Score of 7124 (top 1% of ResearchGate members). I have attracted grant funding from NIHR, MRC, EPSRC, Cancer Research UK, Association for International Cancer Research, British Lung Foundation, Diabetes UK, and many others. I have presented at numerous national and international meetings, particularly around my core research interest of the appropriateness of clinical laboratory testing.
Research and scholarship
Research Interests
Scheduled testing
Around 70% of all clinical biochemistry tests are predictable, routine tests. These scheduled tests fall into 4 categories:
- Monitoring tests in people with long-term conditions (e.g. glycated haemoglobin in people with diabetes).
- Screening tests in high risk groups (e.g. checking for diabetes in women with gestational diabetes or polycystic ovarian syndrome).
- Monitoring the effectiveness of a treatment (e.g. measuring serum levels of lithium in people with bipolar disorder).
- Identification of possible side effects of medications (e.g. monitoring liver function in people such as those with rheumatoid arthritis on disease modifying antirheumatic drugs; DMARDs).
Despite the presence of professional clinical guidelines on the nature and frequency of monitoring in these groups, compliance is often sub-optimal. My research explores the reasons behind this lack of compliance, examines its impact and seeks to find solutions to improve compliance and hence clinical and patient outcomes. The figure highlights the clinical areas of interest and sub-themes in the area of scheduled testing.
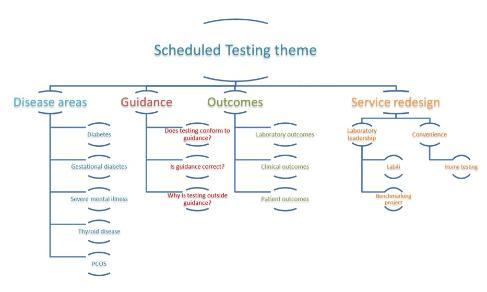
Public and patient involvement
The benefits of involving members of the public in the design, development and delivery of clinical research is increasingly recognised. However, the quality of this public involvement varies considerably both from project to project and organisation to organisation and is frequently tokenistic. We co-produced the NIHR-funded Insight | Public Involvement Quality Recognition and Awards Programme, based on the UK Standards for Public Involvement (UKSPI) alongside an incremental scale designed by Expert Citizens (a lived experience-led community group; see https://expertcitizens.org.uk/insight-public-involvement-quality-recognition-and-awards-programme/), to incentivise and celebrate continuous improvement in public and patient involvement.
Benefits afforded by the programme
We believe that the programme brings together key elements of existing initiatives to create a programme that has several important, often unique, benefits:
Reach & flexibility: It has a very broad geographical reach; it is suitable for national or even international application. It is flexible enough to be applicable to any type of and accommodates any PPIE-active groups from individuals to whole organisations.
Independent, lived experience-led assessment: It provides an independent assessment of public involvement activity, co-led by public contributors, which would assist in validating statements made on grant applications, websites, etc., regarding public involvement activity within an organisation.
Profile: The celebratory nature of the programme’s national annual Awards Event provides the opportunity to raise the profile of public involvement activity.
Spread & Improvement: The Awards Event, along with our plans for a repository of involvement ideas, training and toolkits, facilitate the spread of public involvement activities across health and social care research organisations.
Incentivisation: We feel that our focus on a ‘carrot’ rather than ‘stick’ approach to improving public involvement, by use of an appreciative inquiry approach with celebration of best practice rather than an audit-based programme, is more likely to incentivise participation in the scheme.
Innovation: Our programme encourages innovation in public involvement activities and this is further recognised by the special award for innovation as part of our Quality Awards Event.
Equality, Diversity and Inclusion: Our programme aims to address the general lack of diversity in public contributors, including by encouraging equality, diversity and inclusion in membership of assessment panels and by the use of a special Encouraging Diversity Award.
Impact: Our overall aim is to improve the quality and relevance of health and social care research and we firmly believe that greater public involvement is a key component of this.
Programme workstreams
The development of the programme is progressing through several phases of activity (see figure) with a plan for national roll-out.

Collaborative research
In addition to the two main themes described above, I also work closely with Professor Fahmy Hanna (Professor of Endocrinology & Metabolism) focusing on; (i) gestational diabetes and (ii) adrenal incidentaloma.
Gestational diabetes represents one of the highest risk factors for development of type 2 diabetes mellitus in women. As this increasingly common condition generally affects younger women, early detection of dysglycaemia is key if preventative measures are to be effective. Hence, our research explores approaches to identification of gestational diabetes earlier in the pregnancy, and of type 2 diabetes post-partum in these women, with a view to earlier treatment.
The adrenal incidentaloma (AI) is common and increasing as the use of CT and MRI scans becomes more widespread. However, many AI cases identified by radiologists are not adequately followed up by scan requesters and current processes leave the patient anxious for prolonged periods of time. Our research aims to improve the processes around identification and management of these often neglected patients to enhance patient experience and improve clinical outcomes. We are also examining the biochemical tests used to screen for hormonal over-secretion in these patients with a view to speeding up identification of those with hormonally-active lesions, thereby reducing patient anxiety.
Publications
School of Medicine
David Weatherall building
University Road
Keele University
Staffordshire
ST5 5BG
Tel: +44 (0) 1782 733937
Email: fmhs.facilities@keele.ac.uk
Admissions enquiries: enquiries@keele.ac.uk
The Clinical Education Centre
Keele University
Clinical Education Centre
University Hospitals of North Midlands NHS Trust
Newcastle Road
Stoke-on-Trent
Staffordshire
ST4 6QG
Email us: services.cecreception@keele.ac.uk
CEC general enquires: 01782 731876


